Why The Hard Age Caps On Youth Gender Transition Being Proposed By Conservatives Are A Very Bad Idea
The underlying issues are complicated, but the question of whether these laws make sense isn't even a close call: They don't
Starting late last year, I began looking into a growing conservative trend: the proposal of state laws that would outlaw the administration of puberty blockers and hormones to transgender and gender nonconforming (TGNC) youth. These efforts were picking up steam, and garnered a late-January writeup in the Washington Post. Around that same time, a spokeswoman from Freedom for All Americans, which advocates for LGBT nondiscrimination laws, told me that the organization was tracking state bills in three different categories: bills that would criminalize medical providers for providing these services to minors (in Florida, Missouri, South Dakota, Oklahoma, Colorado, and Kentucky), bills that would subject providers to a loss of their licenses (in Illinois, two in Missouri, and South Carolina), and bills that would label such care as child abuse (in New Hampsire and two in Missouri).
Even before coronavirus hit, these bills were not faring particularly well in terms of actually becoming law. Then, once the pandemic arrived, this issue — like so many others — appeared to take a bit of a back seat. When I checked back in with the FFAA spokeswoman recently, she pointed out that none of these bills had been successful in 2020.
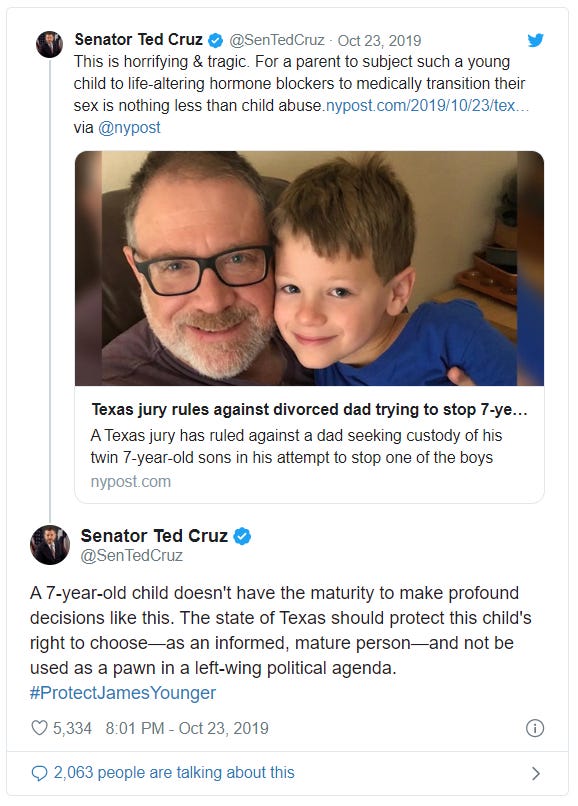
Eventually, though, things are going to return to normal — the culture wars will come roaring back, fiery as ever. And as the issue of youth transition becomes increasingly prominent and politicized, it is quite likely that such state-level efforts will surge once again. These Ted Cruz tweets from October, published in response to a complicated lawsuit in which a father and a mother disagree about whether their child is trans, nicely capture the rising conservative furor over this issue:
“This is horrifying & tragic,” he wrote. “For a parent to subject such a young child to life-altering hormone blockers to medically transition their sex is nothing less than child abuse.” And in a followup tweet: “A 7-year-old child doesn't have the maturity to make profound decisions like this. The state of Texas should protect this child’s right to choose—as an informed, mature person—and not be used as a pawn in a left-wing political agenda.”
Cruz is deeply confused about this subject — a 7-year-old is unlikely to be going on hormone blockers any time soon, and calling what is, at this point, a mainstream medical treatment (and a reversible one) “child abuse” is inflammatory language. But the point is that he represents a growing sentiment among some conservatives: that in fighting youth transition, or at least certain forms of it, they are ‘saving’ children from the evil machinations of liberal activists and doctors and politicians.
While there is an important kernel of truth to some of the concerns over youth transition that is worth discussing — one I’ll get to in the second half of this article — overall, these laws are an extremely bad idea for many rather obvious reasons, and could do serious harm to TGNC youth. They reflect a disturbing attempt on the part of politicians to insert themselves between doctors and their patients. Frankly, they shouldn’t even be on the table — there are far better and less reckless ways to grapple with the genuine complexity underpinning this issue. (The conservative laws being proposed tend to also ban surgeries from being performed on youth who are transitioning. This is a very different issue, and one I’m simply going to punt on — for now it will suffice to say that I’m far more disturbed by the idea of hard age caps on blockers and hormones.)
Before explaining why these laws are so ill-advised, here’s a very quick summary of how the process of youth transition usually works: For a child diagnosed with gender dysphoria at a relatively young age who proceeds to medical interventions, the general trajectory usually starts with social transition (which has no medical component). Then, puberty blockers around the onset of puberty. Then, perhaps a couple years later, if the kid decides s/he really does want to go through with a ‘cross-sex’ puberty (that is, a natal male developing some female secondary-sex characteristics, or vice-versa, which greatly increase the probability they can ‘pass’ as the sex which lines up with their gender identity for the rest of their life, as long as they stay on hormones), they can begin cross-sex hormones. Alternatively, they can stop the blockers and their natal puberty will soon kick in.
There are a number of straightforward problems with setting hard age caps on any step of this process, but perhaps the simplest has to do with the potential health effects of being on puberty blockers for too long. Baked into the general medical consensus that puberty blockers are safe and reversible is the assumption that they’re not going to be used for too long a period. “We do start to worry about the effects of hormone blockers on the bones during a time [young people] should be having rapid accretion of calcium into the bones,” said Daniel Metzger, a pediatric endocrinologist at BC Children’s Hospital in Vancouver, who helped establish that hospital’s protocols for youth transition.
So let’s say a kid who has been competently diagnosed with severe gender dysphoria goes on blockers at 11, but is in, or moves to, a state that passes a ban on cross-sex hormones for anyone who isn’t yet 18 years old. Seven years on puberty blockers would likely be unsafe, and would leave her and her parents in an exceptionally difficult situation where they would either need to move or seek medical care across state lines; halt her blockers, forcing her to endure an involuntary detransition that would likely disrupt her life in numerous ways, complete with a ‘natural’ puberty likely to greatly exacerbate her dysphoria; or somehow have her stay on blockers for a very risky length of time.
Metzger also pointed out that, psychologically, it isn’t ideal for a kid to be in that liminal state for too long. “We want to be sure they are working on their gender journey,” he explained, “not just ‘hanging out.’” And there’s also the simple issue of forcing a kid to wait for very important medical care. “Far and away most importantly,” said Metzger, “there is the fact that these kids are suffering by not having the bodies they need to match their gender. This is a high-risk group in terms of emotional problems, self-harm, suicidal thoughts, etc, etc. At some point you have to look at the risk-benefit of treating kids at age X or maturity level Y, and the risk of not moving ahead with hormones is too great.”
After reaching out to a subset of the gender clinicians I’d relied on to walk me through these issues in the past, including for a long article I wrote in The Atlantic about youth gender dysphoria, I encountered similar sentiments. “We start puberty blocking around the age of 10-12 and start hormones around the age of 15,” said Anna van der Miesen, a clinician at the Gender Identity Clinic at the VU University Medical Center in Amsterdam, which is famous for having pioneered the puberty-blocking protocol and which has produced some of the highest-quality research tracking the trajectories of gender-dysphoric youth over time. “Individualized care is very important in our gender clinic and as clinicians we work together with the youth to see what’s the best for an individual’s development. A hard ban of 18 years would I think undermine the possibilities of individualized gender care.”
Erica Anderson, a psychologist at the UCSF Child and Adolescent Gender Center Clinic who is herself trans, pointed out some of the problems that could be introduced by this sort of top-down state control over medical practice:
As those of us doing youth work with transgender and gender creative kids know the use of ages rather than stages (development) is fundamentally misguided. All youth care involves parental consent. Most of us routinely seek consensus among all those involved: young person, parents, medical professionals and psychological professionals. My colleagues and I always do individualized evaluations. Protocols and guidelines are like guard rails. And to allow legislators to determine what is best for kids is just as onerous as allowing legislatures to decide adult medical care. The professional societies are motivated to offer guidelines based upon the best available science and revise them based upon emerging science and best practices. That is what is happening. The intrusion of lawyers and legislators is not helpful to this process and tends to conflate what people “believe” with what science and professionals “know.”
And Laura Edwards-Leeper, a psychologist at Pacific University who helped bring puberty blockers to the States, and who both sees TGNC clients of her own and trains future clinicians, nicely summed up all the issues at play here in just a couple of paragraphs:
Placing an arbitrary age cap for transgender adolescents who need medical care is not only a poorly thought out idea that runs counter to the [World Professionatl Association for Transgender Health] Standards of Care and [other] clinical guidelines, but I have no doubt that this would put a group of young people who are already at increased risk of severe mental health issues, including suicide risk, at an even greater risk. Such a law would also take the power out of the hands of the mental health and medical providers who are trained to assess and determine each individual child's recommended treatment plan, which is used to optimize outcomes, such as positive psychological health and long-term quality of life for these young people. Providers who are well-trained to do this work recognize that each adolescent is unique, and with a proper assessment, individualized decisions about the best timing for medical interventions can be made in collaboration with the adolescent, parents, and other members of the treatment team.
Another significant problem with implementing age caps is that doing so will likely result in physical complications for some adolescents, specifically those who were started on puberty suppressing medication in early adolescence. Due to a concern about long-term bone health, it is typically not recommended that youth remain on puberty blocking medication too long. Again, each situation is different, but for some adolescents, the medical providers may feel that more than two years on the puberty blockers will increase their risk of bone health problems. Laws such as these would leave the adolescent, family, and doctors no choice but to potentially compromise the child's physical health by keeping them on the puberty suppressing medication until they reach the age at which they were allowed to start gender affirming hormone treatment.
It’s clear, in light of all these issues, that hard age caps on transition run counter to the opinion of many professionals in this area, and that they could cause serious harm. This is a severe instance of lawmakers, many with political agendas and almost all of them ignorant of even the basics of trans healthcare, attempting to interfere with doctors and psychologists who simply want to do right by their patients. Frankly, this isn’t even a close call.
***
But it can simultaneously be true that hard age caps are a bad idea for all these reasons, and that some of the concerns about young TGNC people getting shunted too quickly or too thoughtlessly toward medical treatment are legitimate.
Part of the problem is that there’s a great deal of public ignorance surrounding exactly what a competent assessment process looks like for a kid who might go on blockers or hormones, including the age timeline. As I have pointed out repeatedly in this newsletter and elsewhere, it is shockingly common for major outlets to get various aspects of the gender-identity conversation disastrously wrong, and that includes this particular facet of the issue.
An illustrative example of a mainstream outlet misinforming readers about the timeline issue — and this is one of many — came in an October article in Rolling Stone. In it, EJ Dickson claimed that “under current guidelines gender-affirming hormones such as testosterone and estrogen are not even prescribed for children under the age of 16” (I’m removing a link that didn’t point to any actual guidelines). This is a common claim among those who don’t believe there’s any good-faith discussion to be had here: Youth aren’t actually going on hormones until age 16, so what’s there to worry about?
But the argument is just plain wrong on many fronts. For one thing, neither of the two most important guidelines in this area, WPATH’s Standards of Care or the Endocrine Society’s practice guidelines, explicitly bar cross-sex hormones for those under 16. The former has almost nothing to say on the matter, other than to point out that in many countries 16 is old enough for someone to make their own medical decisions, and the latter notes that “We recognize that there may be compelling reasons to initiate sex hormone treatment prior to age 16 years, although there is minimal published experience treating prior to 13.5 to 14 years of age.” Indeed, many clinics appear to be providing trans youth with hormones and, less often, surgery, well before age 16. The Dutch clinic, mentioned above, is fairly conservative by the standards of progressive American clinics, and as the above email from Anna van der Miesen pointed out, clinicians there give hormones to kids “around the age of 15.” One of the more well-known youth gender clinics in the country, at the Children’s Hospital of Los Angeles, has published studies showing that kids there as young as 12 have been put on hormones, and kids as young as 13 have been referred for double mastectomies.
For all the reasons the above-quoted clinicians and Endocrine Society guidelines lay out, there may sometimes be compelling reasons to not wait until 16 to put a severely dysphoric teenager on hormones, If, that is, the teen in question has gone through a comprehensive assessment process.
But that’s a profoundly important, load-bearing if.
When it comes to a 14-year-old starting cross-sex hormones, for example, there is a massive difference between a situation in which the kid has been under the care of a multidisciplinary gender-clinic team since age 8, and went on blockers at 11, and has been looked after carefully every step of the way, and a situation in which the kid started having a complicated set of mental-health problems, including gender concerns, a couple months ago, and was quickly prescribed hormones without much in the way of mental-health assessment or exploration of their gender feelings.
Many people pretend the latter situation is rare, and for understandable reasons: To acknowledge that it isn’t rare is to make it easier for bad-faith interlocutors to disguise their complete ideological opposition to youth transition as mere medical concern. But at the moment American trans healthcare is a complete Wild West, and whether a given child will have access to a gender clinic at all, let alone a competent one, is a harrowing roll of the dice. In some areas, you might have trouble finding anyone willing to prescribe a young person blockers or hormones; in others you might find recently opened clinics that have very little experience with the difficult developmental issues this line of work brings with it. (And this is all setting aside questions of cost, of course.) This has been pointed out to me over and over by people who don’t have a transphobic bone in their bodies — by clinicians deeply invested in the lives of TGNC kids, many of whom I interviewed for my piece in The Atlantic.
Meanwhile, the same sorts of stories are popping up everywhere: Amidst what appears to be a major worldwide uptick in referrals to gender clinics, clinicians in Canada, the U.S., the Netherlands, Norway, and the U.K. — and probably in other countries, too, that I’m unaware of — have written or told journalists that they are seeing concerning cases that bring them pause, including some in which it’s parents, not kids, driving the push for blockers or hormones. Last year, one of the 15 governors of The Tavistock and Portman NHS Foundation Trust, which helps operate one of the most important gender clinics in the world, in London (with other clinics around the country), resigned amidst the fallout of a damning internal report. As the Guardian summed it up, that report “expressed concern that the service was failing to fully consider psychological and social factors in a young person’s background – such as whether they had been abused, suffered a bereavement or had autism – which might influence their decision to transition.” A handful of staffers have also left the clinic over these concerns. (It should be said that the problems at Tavistock appear to be multifaceted — patients have also complained of unreasonably long wait times, which are also an issue at many American clinics.)
Now, it would be one thing if the clinical guidelines currently in place were being followed. While they aren’t perfect, these guidelines — whether the American Psychological Society’s or WPATH’s or the Endocrine Society’s — all recognize that youth TGNC work is different, and needs to be conducted with even more care, than its adult counterpart. To take just one example, here’s part of what the Endocrine Society had to say on its website about the aforementioned high-profile lawsuit between a child’s father and mother: “As noted in our evidence-based guideline, transgender individuals, both children and adults, should be encouraged to experience living in the new gender role and assess whether this improves their quality of life. Mental health care is recommended throughout this process, and only a mental health professional with training or experience in childhood and adolescent gender development should make a diagnosis of gender incongruence in a child or teenager.”
But there’s strong anecdotal evidence to suggest that these guidelines are often simply being ignored. “When I look at what the [WPATH Standards of Care document] describes, and then I look at my own experience and my friends’ experiences of pursuing hormones and surgery, there’s hardly any overlap between the directives of the SoC and the reality of care patients get,” Carey Callahan, a former trans man and licensed therapist who has since detransitioned and who writes about what she sees as the consistently incompetent care people with gender dysphoria receive in the States, told me for the Atlantic article. (In her case, she is referring to adult care, but the same general issues maintain.) Callahan subsequently helped found the Gender Care Consumer Advocacy Network, which might be the only organization dedicated to ensuring trans and gender-questioning people have access not only to healthcare, but to quality healthcare.
In short, while of course demagogues who have genuine antagonism toward trans people piggyback off these concerns — and use them as a fig leaf for bad ideas like hard age caps — the concerns themselves are legitimate, and it isn’t ignorant bigots raising them: It’s people with a great deal of experience in this area, often firsthand either as patients or clinicians. Anderson and Edwards-Leeper, for example, are both deeply and undeniably committed to helping trans kids get the healthcare they need — as she told me when we got lunch in San Francisco in 2018, Anderson herself was initially denied care when she first sought to transition more than a decade ago, as an adult. But both expressed to me, in my original interviews with them and our followup correspondence for this article, concerns about the lack of consistently followed, rigorous assessment protocols in this area.
“Yes, some kids are not getting sufficient assessments,” explained Anderson in an email (emphasis hers). “The quality of care for trans [people] varies a great deal.” Echoing concerns she expressed to me when we first met, Anderson told me that “Without question providers who are ill prepared to care for trans patients have attempted to do so. Some in my opinion did so because they felt obligated to do the best they could even without adequate training and experience. Others appear to have been opportunistic. Being transgender myself and a psychologist for so many years I see the gains that have been made thanks to WPATH and others. But suddenly trans is trendy and trans people seem like unicorns: fascinating objects of study. When I sense this happening I cringe and it feels very weird.” She doesn’t believe cases of poor youth evaluation are super-rare outliers. “I regularly encounter providers ignorant of the standards of care of WPATH,” she explained. “And assertive/anxious patients who have no tolerance for careful evaluation. It’s a toxic brew.” (In her email, she also noted that it’s perfectly natural and rational that trans people might be skeptical of what they perceive as overly aggressive gatekeeping, given what members of that community have endured in the past.)
Edwards-Leeper pointed out that parents who genuinely want what is best for their kids face a difficult situation if they’re unlucky enough to be in one of the many areas of the country without competent, well-trained youth gender clinicians. “What is problematic is that so many parents these days have reasonable concerns and cannot find a mental health provider who has been adequately trained to assess the gender concerns and ‘readiness’ for irreversible interventions from a psychological perspective,” she explained in an email (emphasis hers throughout). “This results in well-meaning parents being left to make decisions in their child’s best interest without true professional guidance. It puts parents in a horrible position and my heart goes out to them.” She explained that yes, some parents are too skeptical of medical transition, and might wrongly stall their child’s access to blockers or hormones despite a competently conducted diagnosis. “But what about the parents who disagree with the therapist who decided in a 1-hour appointment that their child who came out last week as trans after stumbling upon a YouTube video is ready for testosterone?” Like Anderson, Edwards-Leeper does not believe these cases are extreme outliers. Rather, she has heard from hundreds of parents in these sorts of situations since she was featured in my Atlantic article. “These are the parents who I have banging down my door still, since the Atlantic article,” she explained. “I can’t tell you how many times I'm almost in tears about the state of this field when I get off the phone with them.”
If clinicians who are dedicated to helping trans youth are quitting one major clinic over their concerns in Britain, and are expressing on-the-record qualms about the standards of care in the U.S. and elsewhere, and their positions are clearly laid out, drawing not on bigotry or ignorance but well-established findings in developmental psychology as well as their own considerable professional experience, then it would probably be a good idea to listen to them. That doesn’t mean the answer is to have lawmakers who do have ulterior motives swoop in and tie the hands of competent clinicians in a way that could hurt TGNC youth — again: age-cap laws are a terrible idea.
But it would also be foolish to pretend that unless you’re a transphobe, there’s nothing to discuss here.
Questions? Comments? Derailing tactics? I’m at singalminded@gmail.com or on Twitter at @jessesingal. The lead photograph of a pro-LGBT demonstration is by Denin Lawley, via Unsplash.


If, as you yourself acknowledge, the concerns are real, why do you assume that the lawmakers who are promoting these laws are motivated by straight up bigotry and maliciousness?
I agree it's concerning if, say, you have someone aged 11-13 who abruptly starts having gender issues for a few months and dominant progressive attitudes (and possibly "cis privilege" guilt) pressure the parents to shop around for a clinic that will fast track hormone replacement. The main problem is that gender clinics in many areas are a "wild west" of inconsistent philosophies and practices, so the solution is effective regulation and professional guidelines rather than panic-oriented bills supported by conservative politicians.